Why Patellar Simulation Matters in TKA – And How It Improves Patient Outcomes
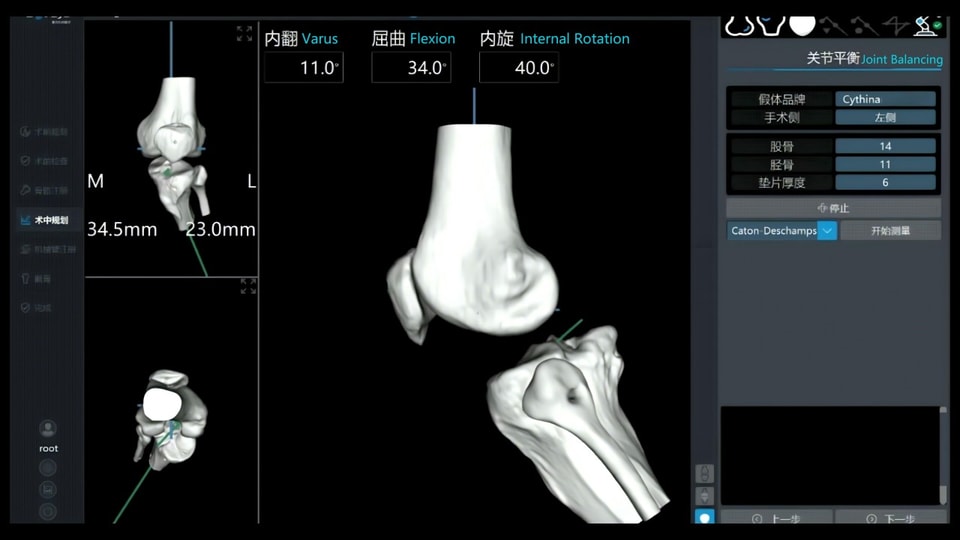
Why Patellar Simulation Matters in TKA – And How It Improves Patient Outcomes
When we talk about success in total knee arthroplasty (TKA), the conversation often centers on alignment, implant longevity, or soft tissue balance. But there's one factor that silently determines whether a patient walks out of the hospital satisfied or frustrated: the patellofemoral joint.
A forgotten patella can undo an otherwise perfect knee replacement. That's why patellar simulation—the ability to virtually model and predict patellar tracking and contact forces before a single bone cut is made—has moved from a "nice-to-have" to a clinical necessity.
The Clinical Problem We Can't Ignore
Anterior knee pain remains one of the most common complications after TKA, affecting up to 20–30% of patients in some studies. It leads to dissatisfaction, revision surgeries, and increased healthcare costs. The root cause? Often it's a mismatch between the implant geometry and the patient's native patellofemoral biomechanics.
Traditional surgical planning tools treat the patella as an afterthought. But every patient has a unique patellar height, trochlear groove morphology, and Q-angle. Without patient-specific patellar simulation, we're essentially guessing how the patella will track post-operatively.
How Patellar Simulation Changes the Game
Patellar simulation allows the surgical team to:
- Visualize patellar tracking in real-time across the full range of motion—from extension to deep flexion.
- Identify potential "overstuffing" or "undercutting" of the patellofemoral compartment before making irreversible bone resections.
- Optimize implant rotation and femoral component sizing to restore the native trochlear groove.
- Reduce lateral retinacular release rates by proactively balancing patellofemoral forces.
The result? A smoother postoperative recovery, less anterior knee pain, and a knee that feels more natural to the patient.
The Value Proposition for Surgeons and Hospitals
For surgeons, patellar simulation reduces intraoperative guesswork and revision risk. For hospitals and healthcare systems, it contributes to higher patient satisfaction scores, shorter lengths of stay, and lower 90-day readmission rates—key metrics in value-based care models.
And for the patients? They get back to hiking, kneeling, and playing with their grandchildren without that nagging anterior pain.
Looking Ahead: Simulation as the New Standard of Care
We are entering an era where predictive biomechanics will define surgical excellence. Just as pre-operative templating for hip replacements became universal, patellofemoral simulation is on its way to becoming a non-negotiable step in modern knee surgery.
In your practice, what is the biggest hurdle in managing patellar tracking? Experience or technology? If you've seen the impact of simulation in your practice, or would like to explore this technology further, let's start a conversation.
Contact Us
Services
Contact Details
Room 4010, 4th Floor, Building 2, No. 8 Gaoshun Road, Wuchang Street, Yuhang District, Hangzhou, Zhejiang Province,China