
News
- Newest
- Oldest
- Name A-Z
- Name Z-A
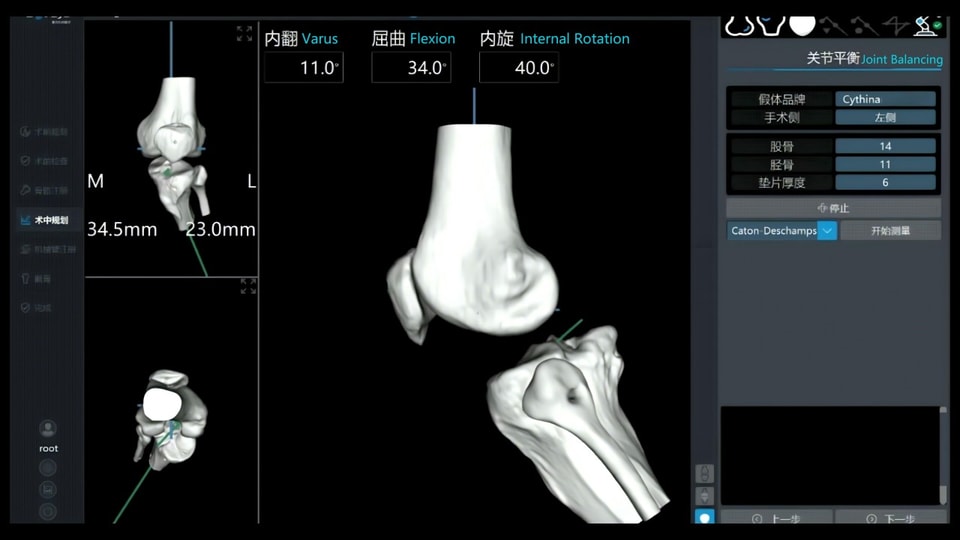
Why Patellar Simulation Matters in TKA – And How It Improves Patient Outcomes
When we talk about success in total knee arthroplasty (TKA), the conversation often centers on alignment, implant longevity, or soft tissue balance. But there's one factor that silently determines whether a patient walks out of the hospital satisfied or frustrated: the patellofemoral joint. A forgotten patella can undo an otherwise perfect knee replacement. That's why patellar simulation—the ability to virtually model and predict patellar tracking and contact forces before a single bone cut is made—has moved from a "nice-to-have" to a clinical necessity. The Clinical Problem We Can't Ignore Anterior knee pain remains one of the most common complications after TKA, affecting up to 20–30% of patients in some studies. It leads to dissatisfaction, revision surgeries, and increased healthcare costs. The root cause? Often it's a mismatch between the implant geometry and the patient's native patellofemoral biomechanics. Traditional surgical planning tools treat the patella as an afterthought. But every patient has a unique patellar height, trochlear groove morphology, and Q-angle. Without patient-specific patellar simulation, we're essentially guessing how the patella will track post-operatively. How Patellar Simulation Changes the Game Patellar simulation allows the surgical team to: Visualize patellar tracking in real-time across the full range of motion—from extension to deep flexion. Identify potential "overstuffing" or "undercutting" of the patellofemoral compartment before making irreversible bone resections. Optimize implant rotation and femoral component sizing to restore the native trochlear groove. Reduce lateral retinacular release rates by proactively balancing patellofemoral forces. The result? A smoother postoperative recovery, less anterior knee pain, and a knee that feels more natural to the patient. The Value Proposition for Surgeons and Hospitals For surgeons, patellar simulation reduces intraoperative guesswork and revision risk. For hospitals and healthcare systems, it contributes to higher patient satisfaction scores, shorter lengths of stay, and lower 90-day readmission rates—key metrics in value-based care models. And for the patients? They get back to hiking, kneeling, and playing with their grandchildren without that nagging anterior pain. Looking Ahead: Simulation as the New Standard of Care We are entering an era where predictive biomechanics will define surgical excellence. Just as pre-operative templating for hip replacements became universal, patellofemoral simulation is on its way to becoming a non-negotiable step in modern knee surgery. In your practice, what is the biggest hurdle in managing patellar tracking? Experience or technology? If you've seen the impact of simulation in your practice, or would like to explore this technology further, let's start a conversation.

Beyond the Closed Loop: The Strategic Shift Toward Open-Platform & Sub-Millimeter Precision in Orthopedics
The rapid proliferation of robotic-assisted total knee arthroplasty (TKA) has presented surgical departments with a complex array of technological choices. Beyond the initial marketing appeal, the clinical utility of a robotic platform is defined by its mechanical architecture, its execution modality, and its integration into the existing prosthetic ecosystem. This review outlines the critical technical metrics that surgeons and hospital administrators must evaluate to ensure long-term clinical and operational success. 1. The Global Landscape: Architectural Archetypes The current market is bifurcated between established global platforms and emerging high-precision innovators. These systems can be categorized by their mechanical philosophy: Legacy Navigational Systems: Established platforms that focus on alignment and positioning, often utilizing smaller footprints or table-mounted designs. Integrated Semi-Active Platforms: Systems that utilize a dedicated robotic arm to assist or perform the bone resection. Within this category, a new generation of High-Rigidity systems, such as Sovajo, is challenging early industry standards by prioritizing mechanical stability as the foundation for accuracy. 2. Critical Evaluation Metrics for Surgical Procurement I. Registration Accuracy: The Sub-Millimeter Frontier While the first generation of robotic assistants established an industry standard accuracy of approximately 0.3 mm to 0.5 mm, engineering advancements have pushed the frontier further. Clinical Relevance: Surgeons should distinguish between "static planning accuracy" and "active registration precision." Newer high-rigidity platforms have documented a registration precision of 0.15 mm. This reduction in the margin of error is vital for complex cases where bone morphology is distorted, ensuring the physical execution matches the digital plan with the highest possible fidelity. II. Execution Modality: Semi-Active Systems vs. Passive Navigation A fundamental distinction lies in how the robot interacts with the surgical tool: Passive Navigation (The "Robotic Jig"): The robot positions a cutting guide, but the surgeon manually operates the saw. While this ensures alignment, it offers no protection against manual deviation or soft tissue injury during the cut. Semi-Active Execution (Integrated Tooling): Advanced platforms utilize a robotic arm that directly controls the instrument (e.g., an oscillating saw). III. Mechanical Philosophy: High-Rigidity vs. Flexible Arm Architectures The physical build of the robotic arm significantly impacts its performance under the stress of bone resection: Flexible/Lightweight Arms: Often designed for portability, these arms may require invasive leg-fixators to compensate for potential movement and lack of inherent resistance during the cut. High-Rigidity Arms: By utilizing a heavy-duty, high-rigidity arm, systems like Sovajo eliminate micro-vibrations during active cutting. IV. Ecosystem Architecture: Open Platform vs. Closed Loop The choice between proprietary and agnostic systems is a primary driver of long-term ROI: Closed Systems: These are tethered to a specific manufacturer’s proprietary implants. While integrated, they limit the surgeon’s clinical choice and can increase the hospital’s supply chain vulnerability. Open Platforms (Implant-Agnostic): Emerging leaders are adopting an open-platform philosophy. Synergy: A system compatible with multiple leading implant brands (various international lines) allows the hospital to leverage its existing inventory. This protects distributor margins and allows for patient-specific implant selection without robotic constraints. Conclusion: Defining the Future Standard For a surgical department, the ideal robotic investment is one that offers a "no-compromise" approach to execution. A platform that combines sub-millimeter precision (0.15 mm), the active safety of a semi-active system, and the mechanical stability of a high-rigidity arm represents the current pinnacle of orthopedic engineering. When these features are housed within an open-platform architecture, the result is a system that enhances clinical outcomes while maintaining maximum operational flexibility.
Revolutionizing Joint Replacement: Why "Rigidity" is the New Gold Standard in Orthopedic Robotics
For years, orthopedic surgeons have embraced robotic assistance to improve TKA/THA outcomes. However, many early-generation systems brought their own set of clinical frustrations—specifically those utilizing "Flexible/Lightweight" robotic arms. The Common Surgeon Pain Points: ❌ Precision Instability: Flexible arms often suffer from micro-vibrations during active bone cutting, leading to osteotomy errors that can exceed 2-3mm. ❌ Procedure Complexity: To compensate for arm flexibility, these systems require invasive leg fixators/immobilizers to ensure the patient doesn't move an inch. This adds surgical time, increases soft tissue trauma, and complicates the workflow. ❌ Predictability Issues: Inconsistent rigidity means inconsistent results. The Sovajo Solution: Engineering Stability with High-Rigidity Arms 🎯 At Sovajo, we believe the robot should adapt to the surgeon, not the other way around. Our next-generation system utilizes a High-Rigidity Medical Robotic Arm combined with proprietary motion control algorithms to solve these legacy issues: ✅ Sub-Millimeter Precision: Our rigid arm minimizes fluctuations to ✅ Fixture-Free Workflow: No more cumbersome leg fixators. The stability of our system allows for a more natural, streamlined procedure that saves valuable OR time. ✅ Integrated Efficiency: With the power saw built directly into the rigid arm, you get a seamless, "integrated positioning and osteotomy" experience. Precision shouldn't come with the cost of complexity. It’s time to move beyond the limitations of flexible systems and embrace the power of Rigid Stability. 🚀 Discover the Sovajo difference. Experience the future of Orthopedic Surgery. #Orthopedics #SurgicalRobotics #MedTech #TKA #JointReplacement #HealthTech #Sovajo #DigitalHealth #OrthoSurgeon #Innovation #SoutheastAsiaMedTech
Categories
Contact Us
Services
Contact Details
Room 4010, 4th Floor, Building 2, No. 8 Gaoshun Road, Wuchang Street, Yuhang District, Hangzhou, Zhejiang Province,China
